Monkeypox, a rare disease similar to smallpox, has been declared a public health emergency. Experts at the School of Medicine at the University of California, Riverside, answer some of the biggest questions surrounding this disease that is affecting an increasing number of people in Riverside County. Information for the UC community is also available.
Brandon Brown, professor of social medicine, population, and public health
Q. What is monkeypox and what are its symptoms?
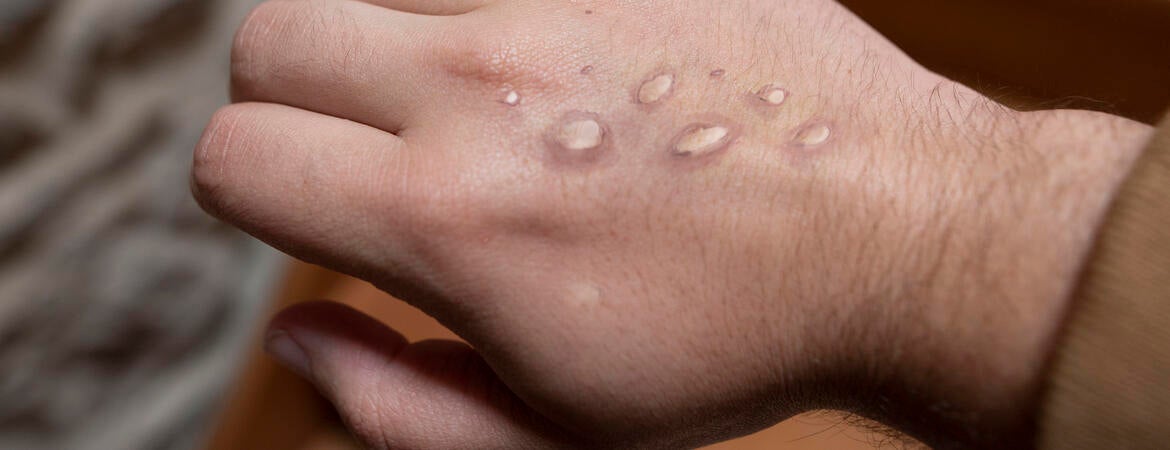
A. Monkeypox is a virus that was first reported in humans in 1970, but which is now a national public health emergency in the United States. Symptoms primarily include a rash on the face, chest, feet, chest, or genitals that looks like blisters and is itchy. Other symptoms include flu-like symptoms, fever, chills, swollen lymph nodes, headache, or respiratory symptoms. Symptoms can last 2-4 weeks.
Q. How does it spread and which communities are at risk?
A. Monkeypox can be spread by close skin-to-skin contact with someone who has monkeypox symptoms (hugging, kissing, massage, sex, or other direct contact), by touching objects used by someone with monkeypox, or by respiratory secretions. Similar to COVID-19, Black and Brown people are more highly impacted by monkeypox. Most current cases are among adult men, but all communities are at risk.
Q. Are children at risk of getting monkeypox?
A. Yes, everyone is at risk of getting monkeypox, and there are cases among children.
Q. Is there a cure?
A. There is currently no cure for monkeypox, but there are medications for symptom management. The majority of symptoms are non-life-threatening.
Q. How can you protect yourself? Do you foresee a larger outbreak?
A. I suggest getting the two-dose vaccine once it becomes available to you; currently the vaccine supply is limited. Wash your hands frequently and avoid skin-to-skin contact with people who are symptomatic with monkeypox. Also, the CDC recommends limiting your number of sex partners. I do foresee a larger outbreak coming, since this is spread by skin-to-skin contact and schools are back in session after the summer break. There is a long incubation period between infection and symptoms, which makes it difficult to know the true number of current cases.
Q. Should you develop symptoms, how do you get tested? If testing is not available, what are the options?
A. There are tests available for monkeypox, and currently people need to have a rash with fluid filled lesions to get a test. If you have symptoms, contact your primary care physician. Isolating from others can prevent the spread of monkeypox; so avoid close contact and use prevention practices, including avoiding travel and public transportation until you are no longer symptomatic.
David Lo, distinguished professor of biomedical sciences
Q. Is a vaccine the best protection? Who should get the vaccine?
A. There are two vaccines available, and in general vaccines are the best protection. These vaccines have been available for several years (ACAM2000 since 2007, MVA-BN versions used in the late 1970s) and were previously approved for prevention of smallpox infection. While their use has been approved, their effectiveness against monkeypox is still being studied. The vaccine should be given to people at high risk for occupational exposure to the virus, such as laboratory workers doing diagnostic testing, but routine vaccination of all healthcare workers is not currently recommended. People with known exposure should consider vaccination within 4 days of the exposure; while it may reduce the symptoms of disease it might not prevent onset of disease. Others who may consider vaccination include those with risk factors that make them more likely to have been exposed (even in the absence of documented exposure to a confirmed case).
Q. How does the vaccine work? Are two shots needed?
A. The two approved vaccines presently available were originally developed to prevent infection from smallpox; vaccination was critical to the eradication of smallpox globally by 1980. The vaccines, JYNNEOS (MVA-BN), and ACAM2000, are both derived from vaccinia virus, which is related to both monkeypox and smallpox; they all belong to the group of viruses called orthopoxvirus. The JYNNEOS virus cannot replicate in humans, and it requires two doses subcutaneously, 28 days apart. The ACAM2000 virus will replicate in humans, and only requires one dose, but it can induce more adverse reactions than JYNNEOS.
Q. How long does the virus last in the body?
A. The time from exposure to monkeypox virus to symptoms ranges from 5 to 21 days, and the symptoms, which are similar to chickenpox (fever, swollen lymph nodes, blisters that crust over) typically last two to four weeks. Risk of death is between 0% to 11% depending on virus variant and location, but secondary infections (pneumonia, sepsis, etc.) and other complications are possible, and if infected during pregnancy, still birth or birth defects can occur.
Nina Grace Ruedas, behavioral scientist, UCR Family Medicine Residency Program
Q. How can anxiety surrounding the monkeypox virus be dealt with?
A. What I offer in this Q&A is not therapeutic advice. For therapeutic advice, please consult a professional.
I suggest labeling the emotions you are experiencing. Research suggests that naming your emotions can act as an implicit form of emotional regulation. This approach also promotes self-awareness and can help you identify next steps.
Although some emotions are difficult and uncomfortable, the goal is not to avoid all negative emotional states. Lower levels of anxiety can motivate you to find resources and advocate. Should anxiety intensify, become excessive, and cause great distress, it may be time to try something different. Short meditations can produce great benefits by helping you be present and lowering your resting heart rate. There are several apps available to support a meditation practice.
Another good strategy is to ask for help. Asking for mental health support from a physician or mental health provider is an act of courage and empowerment. Clinicians and psychotherapists can link you to resources, teach you valuable coping skills, and listen without judgment.
Q. How can someone who has monkeypox be helped?
A. If you wish to help someone who has monkeypox, start by familiarizing yourself with the CDC recommendations. It is important to keep yourself protected and healthy. Then directly communicate your wishes to help. If you know someone who is isolating after a monkeypox diagnosis, they may need groceries or other supplies. Or they may feel alone during the isolation process. Reminding someone that you are one phone call away might be all that is needed. Since everyone’s needs are different when ill, check in with the person directly. The best way to learn how you can best support others is by asking. Direct communication is key.
Q. According to the CDC monkeypox recommendations, I should limit my number of sexual partners. Is this true?
A. Sex is an important part of overall health and wellness. Although monkeypox is not a sexually transmitted infection, it can be transmitted through skin-to-skin contact. Until vaccines are more readily available, limiting your number of sexual partners can be one strategy to reduce your risk of exposure. Recently, the CDC published monkeypox-specific safer sex recommendations.
Q. What are your suggestions for coping with unpleasant memories of the AIDS crisis triggered by monkeypox?
A. Since there are some parallels, monkeypox has triggered unpleasant memories of the AIDS crisis for many. If you find it helpful to have your thoughts and feelings normalized, try talking to people who share similar life experiences. Others who lived through the AIDS crisis might be able to validate your feelings. It might also be helpful to talk to an LGBTQ+ knowledgeable psychotherapist who can listen and suggest coping skills tailored to your needs.
Header image credit: MarioGuti, iStock/Getty Images Plus.